- All posts
- 8 Media Venture
- althetics
- aMMP8
- Annimari Korte
- Antibiotic resistance
- Apotek Härtat
- Aqua Dental
- athlete
- Award
- Baltics
- Bonnier
- Bonnier News
- Brain health
- Business
- Cancer
- cardiovascular disease
- caries
- Chemo therapy
- children
- collaboration agreement
- Croatia
- Denmark
- Denta
- Dental erosion
- Dentex
- diabetes
- Dual Light
- Duodecim
- EFP
- EFR
- Estonia
- EuroPerio
- event
- Expodental
- FIBO
- fund raising
- general health
- Gingivitis
- Gum disease
- HAP
- HealthHub Pharma
- HIDES
- Hospital infections
- hospital-acquired pneumonia
- IBD
- Iceland
- IDS COLOGNE
- implantology
- invest
- investment
- italy
- Koite Health
- Latvia
- Lithuania
- lumoral
- Lumoral App
- Lumoral Junior
- Maritime industry
- Media
- MegaGen
- Movie
- News
- Nordic markets
- Nordics
- O
- Olympics
- Oral health
- Oral hygiene
- Oral mucositis
- Patent
- PDT
- peri-implantitis
- Perio Master Clinic
- Periodontitis
- periodontology
- Photodynamic therapy
- Press
- Ranking
- Romania
- Scandinavian Society of Periodontology
- Science
- Seafarer
- Seedtable
- share issue
- Shareissue
- Siblings movie
- Spain
- spots
- Stroke
- Study
- sweden
- Tartar
- techtour
- Thailand
- UK
- United States
- Valentine's Day
- WHO
- World Cancer Day
- World Health Day
- World Heart Day
- world oral health day
- World Smile Day

Periodontitis and Diabetes: The Connection Between Two Common Diseases
Periodontitis and diabetes are two prevalent diseases with a strong bidirectional relationship between them. Poorly managed diabetes promotes the progression of periodontitis and complicates its tr...

Dental disease that many overlook – this is what you should check for
An untreated inflammation in the gums can eventually lead to periodontitis. Yet, many people overlook the symptoms of gingivitis, as it is also called. Here are the signs you should be on the looko...
Treatment of Periodontitis in Smoking Patients with the Lumoral Method
(This article is based on the writing of dentist Viktoria Ljutkina, published in the largest dental medicine periodical in Estonia, Ajakiri Hambaarst. Ljutkina works as a dentist at Läänemere Hamba...
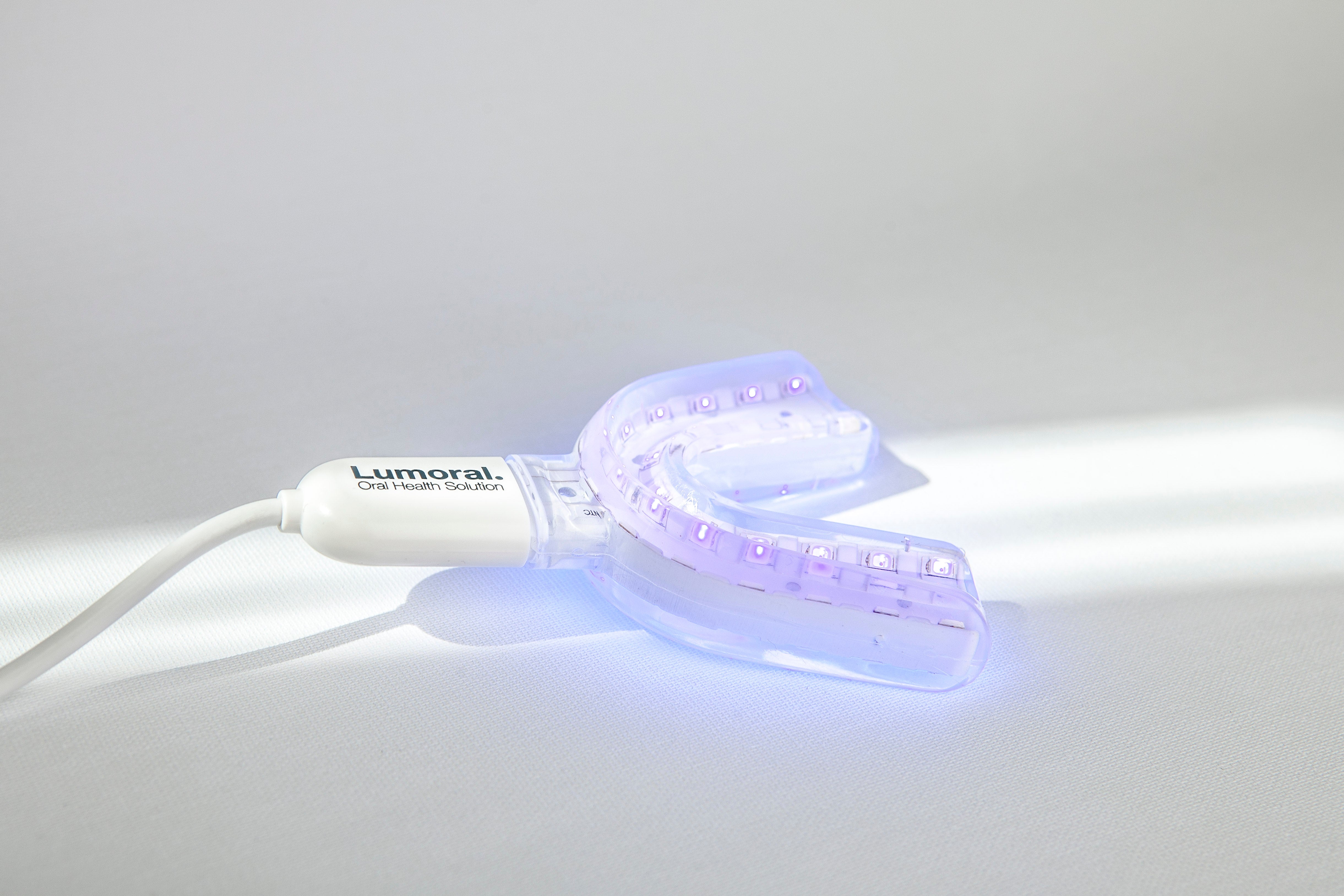
Antibacterial Dual-Light Therapy: A Novel and Effective Approach to Managing Oral Mucositis
Jessica Hentilä, a student at the Faculty of Medicine, University of Helsinki, conducted in-depth research on oral mucositis and its treatment. Oral mucositis is an inflammatory condition of the or...

Poor Oral Health and Oral Dysbiosis: A Link to Systemic Diseases and Cancer
Scientists have discovered a significant link between poor oral health and systemic diseases, including specific cancers. This connection is centered around so-called oral dysbiosis, a condition wh...
Finnish health technology company Koite Health Oy has signed a distribution agreement with Dental Warehouse Ltd. of the UK. Following the accord, Dental Warehouse will offer UK consumers and oral h...